With its strong University heritage, Oxford is home to some of the world’s leading healthcare innovators. And considering Fruto is based in Oxford, it’s perhaps not surprising that healthcare is an area we find ourselves particularly well suited to.
We’re in the fortunate position to have worked on numerous healthcare projects, medical imaging in particular. Our work in this area spans a wide range of specialities, covering software for hearts, lungs, kidneys, brains, bones, dentistry, and even pets (vets).
In this article, we’re going to take a deeper dive into designing medical imaging software that works alongside hardware devices such as MRI and CT scanners, X-rays and ultrasounds - and why user research plays such an important part.
4 key medical imaging software design considerations
Although there are some fairly common design challenges present across all healthcare projects, we’ve identified 4 key areas that need particular consideration when it comes to medical imaging software:
Users’ environment and workflows
Hardware/data input device
User interface design
Patient wellbeing
User environment & clinician workflows
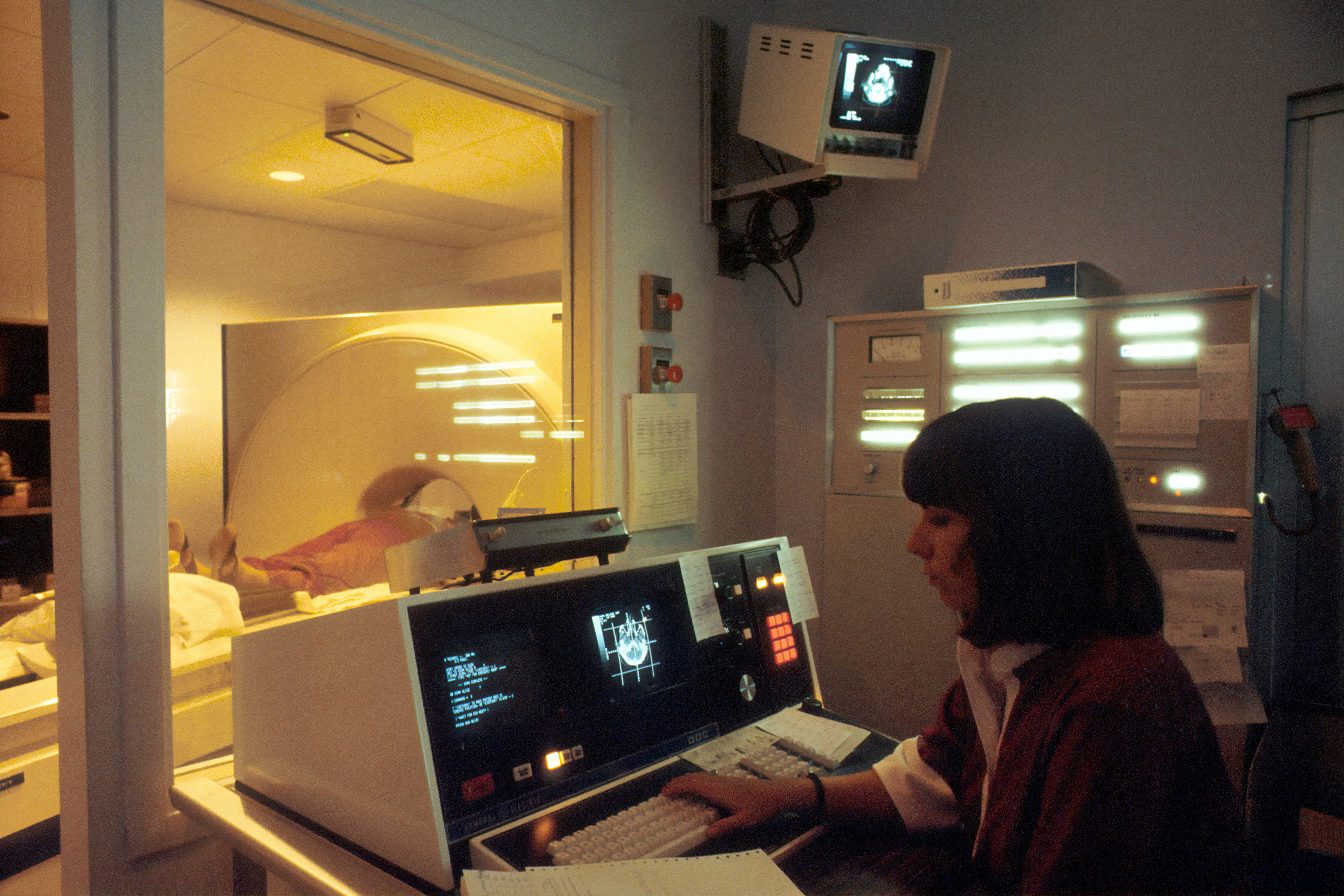
One of the biggest factors we need to take into account when it comes to imaging devices is the clinician’s workflow, especially when using multiple machines, where their workflow may see them moving between where the patient is and with a computer or device (which may be in a separate room).
Smaller, more portable devices (such as Doppler scanners) may not require so many steps in the workflow but still have the same challenges when it comes to operating conditions.
Dark rooms impact the contrast levels, colours, and amount of information that can be displayed on the screen.
We also need to consider the time the healthcare professional will need to spend interacting with the device, versus time with the patient. It’s particularly important that the interface is efficient.
For example, screening for heart disease may occur in patients with multiple layers of tissue, so it can take longer to get the necessary images. Also, in a veterinary setting, there is only so long that the animal can be sedated for to run the screening tests, and we also need to account for positioning the animal in the machine.
Other things we need to consider are:
Is the device switched on/ready to go, or does it need booting up?
Is the patient already in the consultation room when this happens?
How long does an appointment (usually) last?
How many medical professionals are involved in the process?
Hardware/data input device
As designers, we need to remove as much friction from the clinicians’ interactions with the digital interface as possible, so they can focus on taking and analysing the scans as efficiently as possible. As such, the size of the actual imaging device is also important to account for.
Size, shape, and position of the interface can be vastly different from device to device, as can the way the hardware communicates with the interface. For example, the hardware status (“Ready to scan”, “waiting”, “scanning”, etc.) can vary across different medical devices, and we need to ensure we use consistent terminology and colours in relation to the specific hardware the interface is being designed for.
Whether the device is interacted with using a mouse or touchscreen also influences the size and location of various touchpoints.
Lots of clinical annotation is needed when it comes to medical imagery, and often multiple images need to be shown simultaneously - both of which provide a challenge when it comes to displaying lots of important information in (often) small interfaces.
As such, it is especially important to consider the workflows within the interface itself:
Does the medical professional need to input the patient’s information, or does the patient’s data get imported from a patient’s electronic record (EPR)?
If they need to input the information manually, what is the minimum required information, and at what stage does it need to get entered on the screen?
Does the clinician need to compare images based on the patient’s history?
What happens with the images afterwards: is it then fed back to a system or saved in the software?
Some interfaces supply data to train artificial intelligence (AI) models, which means the machine may highlight to clinicians areas to investigate further.
User interface design
Medical devices are a highly regulated industry, so when it comes to medical imaging software, much of the information that gets displayed on the screen is defined by regulatory requirements.
This means we might end up with a large amount of information on the screen, and we need to consider the hierarchy of information and layout very carefully.
Although the software being designed may be new, in most cases, the users themselves will have experience in using similar interfaces, so it’s important to understand the conventions used in medical imaging software and to understand and identify the terminology and content that these expert users will be familiar with.
The use of pattern libraries can help to ensure that the overall design is kept consistent, to help reduce friction as the user moves through the scanning process.
Medical imaging is often about detecting diseases early on or early intervention once a diagnosis has been made, so AI and machine learning are often used in medical imaging software.
AI in medical imaging may also help less-experienced users analyse images more accurately rather than relying on experienced consultants - something that’s especially useful in situations such as pregnancy scans in remote developing countries.
The (r)evolutionary use of AI in healthcare
For all the current hype around ChatGPT and other generative AI technologies, nowhere can the truly transformative potential of artificial intelligence and machine learning be seen than in healthcare.
Although still in relative infancy, the use of AI in healthcare has already been found to have many applications and benefits - improving patient care, in particular.
In the early days, the main use case was around the early diagnosis of life-threatening illnesses such as cardiovascular disease and detecting abnormalities that the human eye may miss. But more recently, AI has begun to play an increasingly important role in treatment, too - especially in cases of cancer.
Other recent studies have highlighted the “exciting and potentially game-changing advance” that replacing the traditional dye contrast scanning methods needed to produce clear image scans with new AI-based imaging technology could have.
In fact, the potential for AI in healthcare is so great that NHS England’s Transformation Directorate has its own AI Lab, which is tasked with “accelerating the safe adoption of artificial intelligence in health and care” in recognition of AIs potential to when it comes to prevention, early detection and treatment of disease, and in “helping the NHS to provide better care and faster access to treatment."
We’re excited to see the development of these new technologies and recognise the importance of the role that we play as designers when it comes to ensuring the tech is used to its full potential.
Patient wellbeing
We’ve left it until last, but most important is the need to consider the patient experience when it comes to medical imaging scans.
Anything medical needs to be sensitive to the patient’s emotional state at the time when they are ‘experiencing’ the scanning process, so it’s important to consider how hard it is to actually take the scan(s) and interpret the images.
When designing for healthcare, it is incredibly important to consider all the different user groups that may come into contact with medical imagery itself (not just those operating the devices/taking the scans) - for example:
The person taking the scan (operative/radiologist/consultant)
The clinician/consultant
A GP/other specialist consultants
The patient
Understanding the format or medium through which the images are reviewed and stored is also important.
Although most of our work so far has mostly been around the detection of disease (wherein the scan gets sent to another system, typically the EPR), there are other scenarios - such as pregnancy scans, where there may be a physical printout for the patient to take away with them from the appointment, for example.
Being overweight, pregnant, or sedated poses unique challenges, as do the patient's age and general physical/mental capabilities. Other accessibility considerations - such as patients’ eyesight and hearing, or their first language - may also need to be considered when it comes to labels that are patient-facing.
If the patient themselves has visibility of the images or is present during a consultation, consistency can help to remove confusion and increase understanding of what can often be quite specific medical terminology.
It is also important to remember that it may not be the same person doing the scan each time - so ensuring the software is intuitive and the language it uses remains constant, as this can help to reduce patient anxiety. This is especially so as the choice of wording when discussing results has been found to be an effective way of avoiding common misconceptions of the severity of a diagnosis.
“Qualitative studies show that communicating a diagnosis of ‘CKD’ [chronic kidney disease] to patients can be uncomfortable and unsatisfactory for all concerned, and primary care physicians often face an up-hill battle to retrieve the situation with reassurance”
- Richard Stevens, an Associate Professor at Oxford University’s Nuffield Department of Primary Care Health Sciences.
The labels used within the software might also need to align with an API that is used to integrate the scanning software with other applications. This may be different across healthcare providers - both between and within public and private sectors.
Medical imaging software design starts with user research
As we’ve already touched on above, the importance of knowing exactly what the device set-up and scanning process is, who will be responsible for it, and what actually happens with the imagery produced are all critical pieces of information that need to be accounted for when designing medical imaging software.
Much of the work we have done in medical imaging so far has been around interface design. But healthcare projects, in particular, almost always include some user research to help ensure we understand the needs of the various user groups - both medical professional and patient side - as well as any other specific user groups.
A user research project ensures you have asked the right questions to answer and have the insights necessary to create an effective UI design. Although it may mean additional time and budget are needed at the start of the project - it is cost-effective in the long run as it gives you more confidence in the solutions.
Our ability to run remote user research means that we’re able to gain the necessary research insights regardless of the location or how specialist and specific your user groups may be. For example, we recently worked on a project that saw us recruit specialist radiologists based in the US (via a user recruitment agency) because that’s where the target market was for the product we were working on.
Research considerations
As touched on in the context of the clinician’s workflow section, the physical hardware poses a challenge when it comes to conducting user research because of the need to observe and interview in real terms (i.e. ethnographic simulations of what the scanning workflow looks like).
When conducting remote user research, we need to ensure the workflow of all the stages - device set up/warm-up, scan, etc. - are captured in enough detail. For example, we need to see the hardware that the user is interacting with, as well as the interface that we’re testing on a computer. (Usually, we achieve this by having a representative of the client with the user to set up the research and to hold a mobile phone with a camera pointing at the user.)
The environment is also an important factor to consider when doing user research, as we might be remote, which is especially challenging when there is a physical product as well.
At Fruto, our mission is to help improve people’s lives through better design - and nowhere can we achieve this more than in healthcare. If you’re looking for a user research or design partner for a project you’re working on, we’d love to talk.
Interested in finding out more? Learn more about our services or get in touch to discuss how we can support your next imaging software design project.





